During your stay
In this section, you will find additional information on what will happen during your stay with us, and what arrangements will be made for your rehabilitation following surgery.
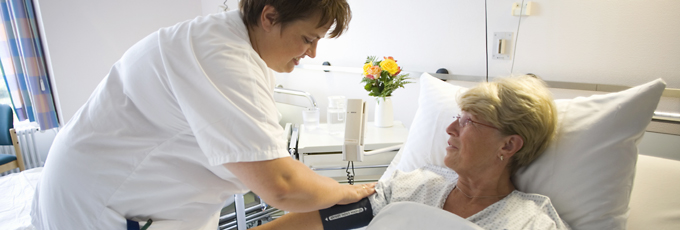
What will happen during your stay in the Department of Heart Surgery?
On the day of your admission, a ward physician will take a detailed medical history. You will also undergo an examination, which will involve having a sample of blood and an x-ray taken. Additional tests may be required, such as a cardiac ultrasound, an abdominal ultrasound or an ultrasound scan of the carotid artery.
The ward physician will explain in detail what will happen during your surgery, and will answer any questions that you may have in relation to this. Your anesthetist will explain to you what type of anesthesia will be required for the procedure and will be happy to answer any questions you may have. If required, our nursing and care staff can administer a mild sedative to help you sleep. On the day of surgery, you will be taken to the operating room shortly after 7:00 am or around midday, depending on the surgical schedule for the day. Once in the operating room, you will be given an anesthetic which will make you go to sleep. The surgeons will then perform the operation.
Depending on the procedure, this can take between 3 to 5 hours. You will wake up in the Intensive Care Unit, where your intubation tube will be removed as soon as you are able to breathe on your own. You will usually need to remain in the Intensive Care Unit for observation until the following morning, when you will be moved to the Observation Unit on Ward 5.
Once here, your mobilization will begin. You will receive assistance that will allow you to sit on the edge of the bed and, later, in a chair. By that time, you will also have started to drink fluids, as well as being allowed to start eating small amounts of food. Depending on the complexity of your procedure and your overall health status following surgery, you will then be moved to the normal ward, where you will gradually start to eat a normal diet, as well as undergoing further mobilization. You will have physicians, nursing and care staff, as well as physiotherapists at your disposal.
Should you have any concerns that you feel our medical staff are unable to help you with, please feel free to speak to one of our psychologists or our pastoral care team (Pastor Ralf-Peter Greif or Lutz Bratfisch).
Preparing for rehabilitation following heart surgery
Approximately 8 days after your surgery, our social worker will be able to assist you in preparing your application for rehabilitation following discharge. There are two possible options:
- You can return home, where you can rest for a few days (approximately 5-14 days) before travelling to the rehabilitation center. This way you will be physically stronger and better able to cope with rehabilitation.
- Alternatively, should you not feel sufficiently confident that you will be able to care for yourself at home, we can arrange for you to be transferred from the hospital directly to the rehabilitation center.
Our experience with our patients tells us that rehabilitation is extremely beneficial and will help to speed up your recovery. However, discharging a patient too soon is associated with increased risks and can hinder recovery.
Most rehabilitation centers offer the option of having your partner stay with you. The costs associated with this option are approximately what one might expect to pay in a reasonably priced hotel.
A further option that is open to you is to be transferred back to your local hospital. This option is usually only considered when the patient is in need of further inpatient treatment but not further surgery, and has proved particularly beneficial for patients who are still quite poorly following surgery, or who have trouble coping on their own.
Patients with diabetes
Diabetes is an important cardiovascular risk factor. Not only do patients with diabetes tend to develop cardiovascular disease earlier but their disease also tends to be more severe.
Patients with diabetes are more likely to develop:
- Early onset coronary artery atherosclerosis
- Atherosclerotic changes affecting several of the coronary arteries (multi-vessel coronary artery disease)
- Stenoses affecting the main stem directly at the site or behind the site where the coronary arteries arise from the aorta (main stem stenosis)
- Stenoses of the more peripheral sections of the coronary arteries
- Complex and more severe stenoses
- Impaired blood flow through an infarct-related artery
Based on the recent literature, researchers are now working under the assumption that patients with diabetes must also have coronary heart disease. As a result, the treatment of patients with diabetes now incorporates the same objectives as the treatment of patients with established coronary heart disease.
Approximately 25-30% of our patients have type 2 diabetes. These patients frequently present with severe coronary artery disease that requires complex interventions or even bypass graft surgery.
The Brandenburg Heart Center supports the campaign for a "Diabetes Excellence Center" that would result in improved hospital care for patients with diabetes.
All our inpatients are screened for diabetes. Upon admission, all patients have their HbA1c levels tested, which allows us to assess their health status in relation to diabetes as well as their overall metabolic health.
Patients who are known to have diabetes receive support from our Diabetes Team throughout their stay.
Our Diabetes Team:
- OA U. Schwill
- N. Jonas, Specialist Advisor on Diabetes, German Diabetes Society
Due to the need for patients to refrain from eating and drinking prior to surgery and/or the administration of contrast agents, oral antidiabetic drugs are usually discontinued for the duration of the patient's stay in hospital.
Our aim during the patient's stay in hospital is to normalize blood sugar levels. This is achieved via a sliding scale regimen for insulin administration, with individual doses depending on the patient's current blood sugar levels.