Electrophysiology procedures for heart failure
Over the past 10 years, electrophysiology procedures have firmly established themselves as a treatment option for patients with heart failure. This development has brought new hope to patients with severe forms of the disease.
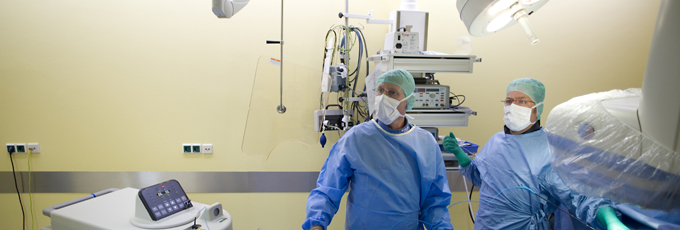
What exactly are electrophysiology procedures for heart failure?
Electrophysiology procedures for heart failure primarily include::
- Cardiac resynchronization therapy (CRT)
- Cardiac contractility modulation (CCM)
- Vagus nerve stimulation (VNS)
For many years, electrophysiology procedures have formed an integral part of the Brandenburg Heart Center's approach to the treatment of heart failure, and the Center has built an enormous amount of experience and expertise in what is still a relatively new area of treatment. By achieving a significant reduction in symptoms, electrophysiology procedures can lead to significant improvements in the patient's quality of life. In many studies, cardiac resynchronization therapy has been shown in many studies to improve patient outlook and survival.
Cardiac resynchronization therapy (CRT)
Since the first case report on a new type of cardiac stimulation was published in the late 1990s, cardiac resynchronization therapy has become an integral part of the treatment approach in a select number of patients with severe systolic heart failure.
In the beginning, this treatment was primarily used in patients who had been diagnosed as having severe heart failure according to the New York Heart Association system of classification (i.e. NYHA classes III and IV), as well as having severe left bundle branch block and severely reduced left ventricular function, or "left ventricular ejection fraction" (LVEF < 35%).
In recent years, physicians have become more experienced in the use of this complex technology and, with the technology increasingly gaining acceptance among the profession, cardiac resynchronization therapy has continued to expand in terms of the range of indications accepted as qualifying for treatment.. Based on research data, current guidelines now recommend CRT even in patients with milder symptoms of systolic heart failure and a broad QRS complex, i.e. patients in NYHA function class II, with an LVEF < 3 5%, QRS > 150ms, normal sinus rhythm and optimal pharmacological treatment (please refer to Focused update - device therapy in heart failure 2010)
The new guidelines, published as recently as 2012, have further expanded the indication for CRT. There is now a clear indication for CRT in patients with mild symptoms (NYHA function class II) and a narrower QRS complex ≥ 130 ms.
In short, any patient with a LVEF < 35%, normal sinus rhythm and a QRS of at least 150ms should receive a CRT device, regardless of their NYHA function class. This type of patient is certain to benefit from CRT.
In patients with severe symptoms (NYHA function class III or above) and a QRS of between 120ms and 150ms, the guidelines suggest that a CRT device may be implanted. In these patients, however, CRT is unlikely to show any real clinical benefit. The therapy planning process for this group of patients may benefit from additional investigations such as MRI (for information on scarring or ischemia) or echocardiography. These may give some indication as to the likelihood of CRT showing clinical benefit. Similar rules apply to patients in NYHA function class II, with a QRS of up to 130ms, for whom the new guidelines have introduced an expanded indication for CRT .
CRT forms an integral part of the specialist treatment provided by the Brandenburg Heart Center's Department of Cardiology. PD (Assistant Professor, non-tenured) Dr. Butter, Head of the Cardiology Department, is one of the pioneers of this modern technique in Germany. He is involved in a nationwide training program that sees him delivering lectures, as well as providing training in CRT.
Approximately 100 CRT devices are implanted every year at the Brandenburg Heart Center. Our state-of-the-art facilities reflect all of the latest advances in implantation technology, allowing our patients to benefit from the considerable improvements that have taken place in the field of CRT device implantation over the past few years.
Cardiac contractility modulation (CCM)
Cardiac contractility modulation offers a new treatment approach that consists of delivering electrical impulses to the heart. As these impulses are delivered during the absolute refractory period of the action potential, premature excitation of certain areas of the heart muscle is prevented. Treatment effect is therefore independent of QRS duration and dyssynchrony. CCM works by delivering electrical impulses that have approximately 100 times more energy than normal pacing impulses during the absolute refractory period of the action potential. Studies have shown that CCM improves exercise tolerance, and therefore quality of life, in patients with severe heart failure.
CCM complements other electrophysiology procedures currently available, providing an option for patients with severe heart failure who have a regular sinus rhythm, and either do not qualify for CRT or have not benefited from CRT. Different experimental and clinical studies have shown CRT to achieve long-term improvements in cardiac contractility, as well as a long-term reduction in the severity of symptoms in patients with heart failure.
The implantation process of the OPTIMIZER III-® IPG (implantable pulse generator) is similar to that of a pacemaker, and is performed under local anesthesia. A total of 3 electrodes are implanted (2 electrodes in the ventricle, one in the atrium).
CCM can also be used in combination with CRT. This particularly applies to CRT "non-responders", i.e. patients who do not benefit, or no longer benefit, from CRT. Although this means that the patient needs to have devices implanted in the infraventricular regions on both sides of the chest, current clinical data do not suggest that the process of implantation becomes more technically challenging as a result. Similarly, there are no data to suggest adverse effects as a result of an interaction between two correctly programmed devices. The majority of patients who are fitted with CCM devices have already been identified as requiring an ICD as part of primary or secondary prevention. Recurrent and persistent supraventricular tachycardia, frequent ventricular extrasystoles, as well as permanent bigeminy and more severe forms of ventricular arrhythmia, represent contraindications to CCM treatment.
In contrast to all other currently available CCM implants, the OPTIMIZER-III-® is powered by a rechargeable battery. The OPTIMIZER-III-® IPG unit is easy to recharge at home and, following appropriate training, patients can recharge the unit once or twice a week. A simple display unit allows patients to obtain information on the charging process, as well as feedback on how well the device is working. The charging process, which takes approximately 90 minutes, does not in any way interfere with the device's programs or settings.
Vagus nerve stimulation (VNS)
Vagus nerve stimulation is currently being investigated in clinical studies, prompted by the fact that increased levels of sympathetic nervous system activity, and reduced levels of parasympathetic nervous system activity, have been associated with increased mortality in patients with myocardial infarction (heart attack) and patients with chronic heart failure.
Autonomic dysregulation with increased sympathetic nervous system activity and reduced parasympathetic nervous system activity is characteristic of patients with heart failure. It is associated with increased morbidity and mortality both in patients with myocardial infarction, as well as in patients with heart failure. Given that pharmacological therapy (beta blockers) has been shown to improve the outlook of patients with heart failure, the question arises as to whether combining this approach with other measures, aimed at correcting sympathoadrenal imbalance through activation of parasympathetic nervous system activity, might be beneficial to patients with heart failure.
Stimulation of the vagus nerve would, therefore, appear to be a logical treatment concept. Following the publication of experimental data and early results from clinical studies, this new treatment concept is currently being investigated as part of larger clinical studies.