PTA for peripheral arterial disease
The term peripheral arterial disease describes a condition that is characterized by impaired blood flow in the limbs, most commonly in the legs. This disease is extremely widespread, and affects over 4 million people in Germany. Depending on the exact location of the arterial stenosis, the disease can be divided into three types, depending on whether it affects the pelvis, thighs or calves.
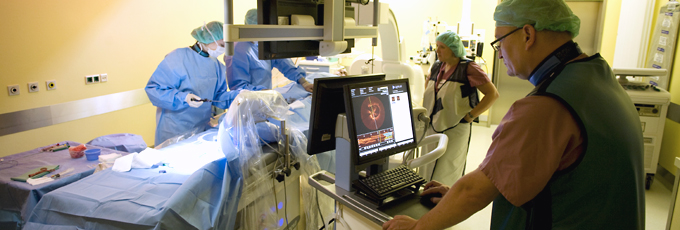
What is PTA for peripheral arterial disease?
Percutaneous transluminal angioplasty (PTA) refers to the use of catheter-based interventions to treat impaired blood flow in the limbs.
In addition to using balloons to dilate narrowed blood vessels, PTA can also include the use of drug-eluting balloons, endovascular stents, and drug-eluting stents. PTA may also involve the use of lasers, aspirators and drills, although this is much less common.
Historical origins and development
Charles T. Dotter and Melvin P. Judkins fathered PTA when they first used a catheter to widen a stenotic blood vessel in 1964.
This technology has undergone - and continues to undergo - considerable developments, and is now regarded as the first-line treatment in patients with peripheral arterial disease (PAD).
What is the purpose of this type of treatment, and what are the results?
One of the basic tenets of PAD treatment is the management of risk factors such as smoking, diabetes, high blood pressure and abnormalities in lipid metabolism.
Although the use of supervised walking programs and medication have proved successful in the treatment of PAD, a catheter-based intervention may be advised in cases where these measures do not achieve sufficient improvements in symptoms or the distance a patient can walk before developing pain.
If the site(s) and extent of the stenosis are such that PTA is unlikely to be successful, bypass surgery should be considered.
- The procedure is performed under local anesthesia.
- Access is usually through the femoral arteries (in the groin). Depending on the site of the stenosis, a small incision is made either on the affected side or the contralateral side. A sheath is inserted into the access site, through which catheters can be introduced.
- Visualization of vessel anatomy is achieved using contrast agents (angiography).
- A balloon placed inside the blood vessel is used to dilate the narrowed section. This may involve the use of a number of balloons of different sizes.
- Often, the decision as to whether stent implantation is necessary can only be made once the procedure is in progress. If this is the case, the stent will be implanted following balloon angioplasty.
- Results are then checked using angiography.
- RThe catheter delivery system and sheath are removed, followed by closure of the access site in the femoral artery.
- A pressure bandage is applied.
Web links
Deutsche Gesellschaft für Gefäßmedizin (German Society of Angiology, DGA)
Leitlinien zur Diagnostik und Therapie der peripheren arteriellen Verschlusskrankheit [guidelines on the diagnosis and treatment of peripheral arterial disease]
http://www.dga-gefaessmedizin.de/uploads/media/