Ablation of AV nodal reentrant tachycardia (AVNRT)
AVNRT is a benign type of arrhythmia that is characterized by fast, regular palpitations that start and stop quite suddenly. Ablation of the faulty electrical pathway has been shown to achieve good results.
Contact
What is catheter ablation for AV nodal reentrant tachycardia?
Catheter ablation is the standard method of treatment for patients who have had several episodes of AV nodal reentrant tachycardia. Ablation of the faulty electrical pathway ("slow" pathway) has been shown to achieve excellent results (>95% success rate), with a normal heart rate being restored. It is rare for AVNRT to recur following successful ablation, with the risk of this happening less than 5%.
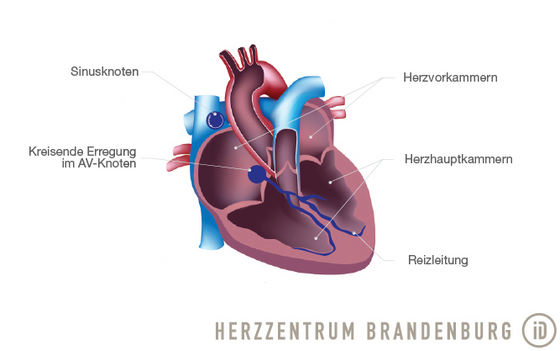
What happens during the ablation of AV nodal reentrant tachycardia?
This procedure consists of the ablation of one of the two electrical pathways in the heart. This ablation of the "slow" electrical pathway has been shown to achieve excellent results (>95% success rate). The greatest risk associated with this procedure is the potential disruption of the electrical transmission of impulses between the atrium and the ventricle (third-degree AV block), which will require the implantation of a pacemaker. However, the risk of this happening is lower than 1%.
Prior to the procedure
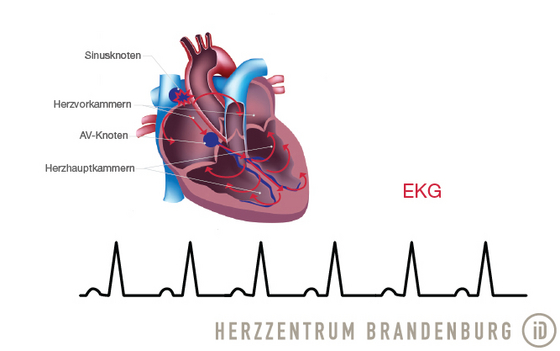
The examination takes place in a specially equipped catheterization laboratory - our electrophysiology laboratory. Prior to undergoing the actual procedure, the patient will be connected to a number of different monitors (e.g. ECG). This allows continuous monitoring of the patient's heart function throughout the procedure.
During the procedure
At the start of the procedure, a local anesthetic is applied - usually on the right side of the groin. Electrophysiology catheters (thin, flexible probes) are introduced into the femoral vein, and advanced to the heart. These catheters are positioned using imaging technology, and can be used to record ECG readings from the inside of the heart.
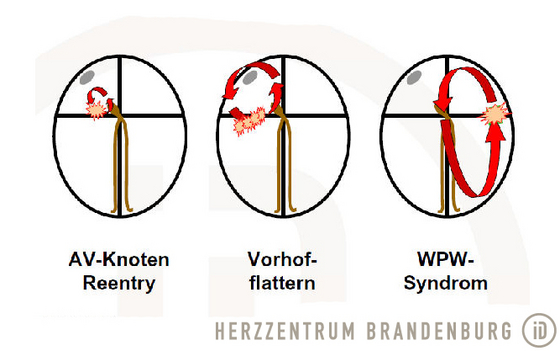
In order to be able to make a definite diagnosis of AVNRT, tiny, imperceptible electrical impulses are administered to trigger the arrhythmia.
Once this has been done, a special catheter is used to ablate the area of the slow pathway by heating it to approximately 50°C, maintaining this temperature for a few seconds. This results in the treated area no longer being able to conduct electrical impulses. After successful completion of the ablation procedure, further testing is carried out to establish whether the arrhythmia can still be triggered. At the end of the procedure, the catheters are removed.

After the procedure
The patient will remain in the catheterization laboratory while a pressure bandage is applied, and will require a few hours of bed rest. After being discharged, patients should try to avoid physical activity for a duration of one week. Recurrence of this form of arrhythmia after successful ablation is possible but rare (risk <5%).
Where can I find out more about the ablation of AVNRT?
Deutsche Herzstiftung e.V. (German Heart Foundation)
Palpitations (racing heart)
herzstiftung.de
Deutsche Gesellschaft für Kardiologie (German Cardiac Society)
dgk.org
