Ablation of typical atrial flutter
Typical atrial flutter is a relatively common type of arrhythmia that is caused by an electrical impulse arising in the right atrium entering a circular pattern between the right atrium and the right ventricle. For years, catheter ablation has been established as an effective treatment method for patients with typical atrial flutter.
Contact
What is catheter ablation for typical atrial flutter?
Catheter ablation is the treatment of choice in patients with recurrent episodes of atrial flutter. This procedure is extremely successful (>95 %) in eliminating the cavotricuspid isthmus, a narrow bridge of fibrous tissue between the inferior vena cava and the tricuspid annulus. Catheter ablation of this part blocks the movement of the electrical impulse, preventing it from entering its circular pattern and thus eliminating atrial flutter.
Development of catheter ablation
For years, catheter ablation has been established as an effective method of treatment for patients with typical atrial flutter.
When should catheter ablation be used in patients with typical atrial flutter?
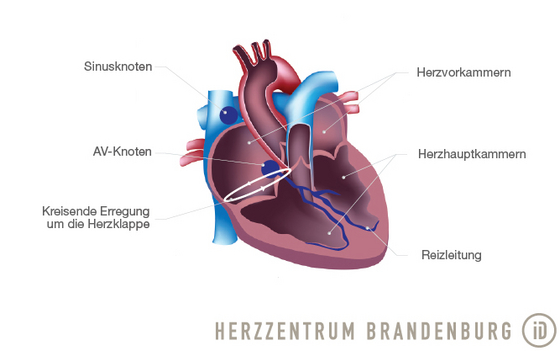
Typical atrial flutter
What happens during the ablation of typical atrial flutter?
Catheter ablation is the treatment of choice in patients with recurrent episodes of atrial flutter. This procedure is extremely successful (>95 %) in eliminating the cavotricuspid isthmus, a narrow bridge of muscle tissue between the inferior vena cava and the lower edge of the tricuspid annulus.
Prior to the procedure
The examination takes place in a specially equipped catheterization laboratory - our electrophysiology laboratory. Prior to undergoing the actual procedure, you will be connected to a number of different monitors (e.g. ECG). This allows continuous monitoring of your heart function throughout the procedure.
During the procedure
At the start of the procedure, a local anesthetic is used to numb the area around the entry site(s), which is (are) usually on the right side of the groin. Electrophysiology catheters (thin, flexible probes) are introduced into the blood vessels and advanced to the heart. These catheters can record ECG readings from the inside of the heart, and are positioned using x-ray guidance.
Once in position, the catheters are used to ablate the cavotricuspid isthmus by heating the relevant area to approximately 50°C. This temperature is maintained for a few seconds, and results in the treated area no longer being able to conduct electrical impulses. Once the relevant area has been successfully ablated, the procedure is often interrupted for a considerable period of time in order to determine whether the ablated tissue is likely to recover. At the end of the procedure, the catheters are removed.
After the procedure
You will remain in the catheterization laboratory while a pressure bandage is applied to the access site. This will need to remain in place for a number of hours (exact duration to be determined after the procedure), which means you will be required to stay in bed. You will usually be able to eat and drink as soon as you are back on the ward. In rare cases, it may be necessary to monitor the patient's heart rate for some time after the end of the procedure.
Discharge from hospital
It is usually possible for patients to be discharged the day after the procedure.
At home
After being discharged, you should try to avoid physical activity for a duration of one week.
Recurrence of this form of arrhythmia after successful ablation is possible but rare.
More information
Deutsche Herzstiftung e.V. (German Heart Foundation)
Palpitations (racing heart)
herzstiftung.de
Deutsche Gesellschaft für Kardiologie (German Cardiac Society)
dgk.org
