Endovascular aneurysm repair (EVAR)
Endovascular aneurysm repair involves the implantation of stent grafts to line and support the aorta. Access for this procedure is usually via the artery in the groin (iliac artery).
Contact
Aortic defects - including aneurysms (enlargement of the aorta) - can place patients at an increased risk of aortic dissection (a tear in the aortic wall), which constitutes a life-threatening situation
An aortic aneurysm that exceeds a certain size, or appears to be growing rapidly, should therefore be stabilized. If the patient is experiencing acute pain, the aneurysm is considered unstable. In this instance, prompt treatment is crucial.
This procedure can be performed using either minimally-invasive techniques (EVAR) or through open surgery. The decision as to which approach is more suitable for a particular patient depends on factors such as the patient's anatomy and concomitant disease, and must be made on a case by case basis.
History and development
The techniques involved in stent implantation were developed in Switzerland during the 1970s. In 1977, Andreas Grüntzig, a German specialist in internal medicine, performed the first-ever successful balloon dilation of a coronary artery in a patient at risk of myocardial infarction. The idea that stabilization of the aorta could be achieved using an expandable wire mesh, was but the next logical step.
Once the first stent graft procedure had been performed in 1991, the procedure continued to undergo rapid development, and quickly became established within the profession. The main benefit of the procedure is that open surgery, and the trauma associated with it, can be avoided.
What conditions are treated with this procedure?
- Thoracic aortic aneurysm (a dilation of the aorta in the chest area)
- Infrarenal aneurysm (an abdominal aneurysm, or dilation of the aorta, below the kidney)
- Aortic dissection (a tear in the inner wall of the aorta)

What does the procedure achieve?
By placing a stent covered with either polyester or PTFE inside the affected vessel, the aneurysm is excluded (it is separated off from the blood flow through the aorta). As the aneurysm is no longer exposed to the pressure (blood pressure) that exists inside the aorta, further enlargement of the aneurysm is prevented, as is the risk of aortic dissection. If an aortic dissection has already occurred, the tear is effectively sealed by the stent, resulting in the stabilization of the affected section of the aorta.
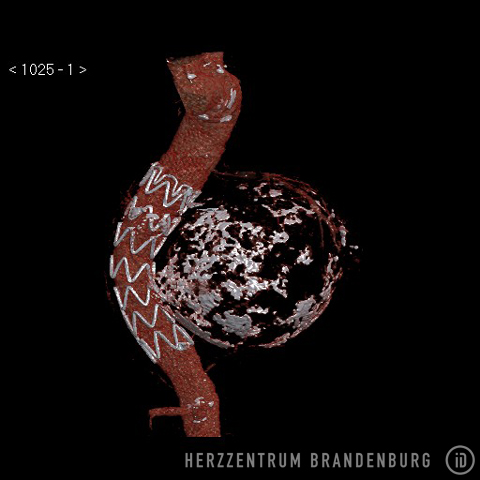
What happens during EVAR?
While the procedure is usually performed under general anesthesia, it is sometimes possible to use local anesthesia. Access is usually through the femoral arteries (in the groin). Depending on the patient's anatomy, access to the arteries is via a small incision in the skin, or following surgical exposure of said arteries. In addition to the access site necessary for the procedure, a further access site has to be established to ensure angiography can be performed throughout the procedure. After preparation of the access sites, the following procedural steps are preformed:
- Visualization of vessel anatomy using contrast agents (angiography)
- Placement of stent using a catheter delivery system
- Release of stent from catheter delivery system
- Monitoring of progress using angiography. Where necessary, a balloon is used to help the stent expand and conform to the artery walls.
- Removal of the catheter delivery system and closure of the femoral artery.
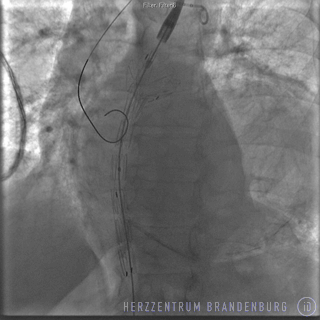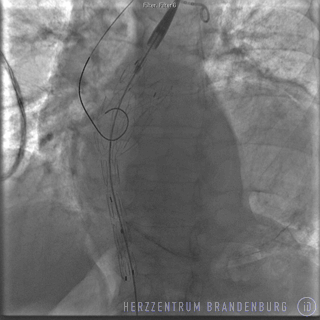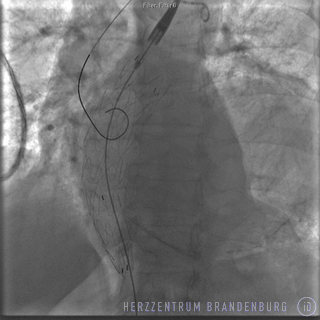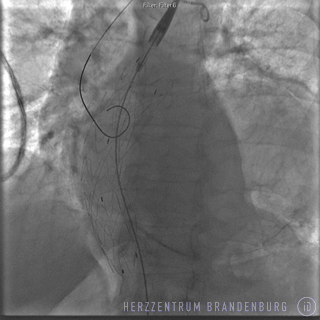
Specialist publications
Guidelines on abdominal aneurysm and iliac artery aneurysm
Deutsche Gesellschaft für Gefäßchirurgie (German Society of Vascular Surgery)
gefaesschirurgie.de
Thoracic Endovascular Aortic Repair (TEVAR) for the treatment of aortic diseases
Association for Cardio-Thoracic Surgery (EACTS), European Society of Cardiology (ESC), European Association of Percutaneous Cardiovascular Interventions (EAPCI)
escardio.org
Clinical Practice Guidelines for Endovascular Abdominal Aortic Aneurysm Repair
Society of Interventional Radiology
sirweb.org
